For health plans: every member call, scored. Every grievance, found.
100% conversation coverage on member services. HIPAA-aware redaction. Real-time agent guidance for benefits, prior auth, formulary, and appeals. Voice of the Member that surfaces network-adequacy complaint trends before CMS does, and helps you protect Star Ratings before bonus season.
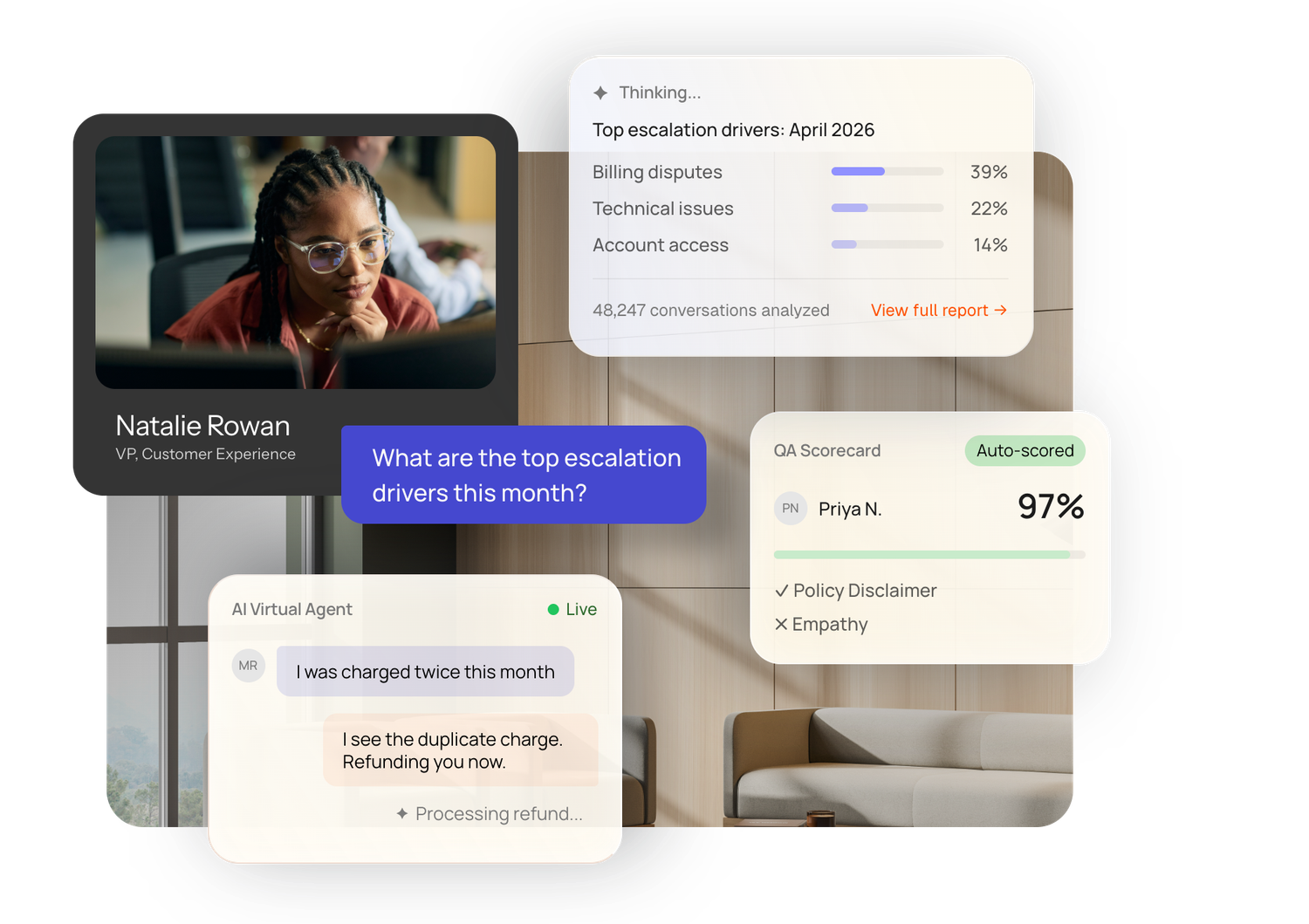


















From every member call to a Star Ratings outcome.
Level AI turns every member interaction into HIPAA-aware context that drives faster appeals resolution, fewer grievances, higher member CSAT, and the Star Ratings posture that protects MA bonus payments. Each 0.5 star is roughly $300 PMPY for Medicare Advantage plans, and member experience signals make up nearly half the weighted score.
Trusted by leading member services organizations
Level AI was the change we needed for member services. We doubled the productivity of our QA team, lifted member CSAT on appeals and benefits calls, and finally have HIPAA-aware visibility into the conversations that move our Star Ratings.

The PHI redaction and member call screen recording won the day. Our compliance team signed off on the deployment in weeks, not quarters, and our competition said they just couldn't match Level AI on HIPAA-aware QA.

As a national health plan, member experience is everything we are measured on. Level AI's agent screen recording has added eyes to a process where we only had ears before. We can identify exactly where reps stumble on prior auth and formulary, coach them on member empathy, and watch our CAHPS-style scores climb.

We get so much intel about our member calls that it has reshaped how we run grievance and appeals. We've gone from manually scoring 1-2% of member calls to using Level AI to score 100% of them, and the operational signals we surface now reach the executive team weeks before they would have shown up in CMS data.

Level AI was the change we needed for member services. We doubled the productivity of our QA team, lifted member CSAT on appeals and benefits calls, and finally have HIPAA-aware visibility into the conversations that move our Star Ratings.

The PHI redaction and member call screen recording won the day. Our compliance team signed off on the deployment in weeks, not quarters, and our competition said they just couldn't match Level AI on HIPAA-aware QA.

As a national health plan, member experience is everything we are measured on. Level AI's agent screen recording has added eyes to a process where we only had ears before. We can identify exactly where reps stumble on prior auth and formulary, coach them on member empathy, and watch our CAHPS-style scores climb.

We get so much intel about our member calls that it has reshaped how we run grievance and appeals. We've gone from manually scoring 1-2% of member calls to using Level AI to score 100% of them, and the operational signals we surface now reach the executive team weeks before they would have shown up in CMS data.

Level AI was the change we needed for member services. We doubled the productivity of our QA team, lifted member CSAT on appeals and benefits calls, and finally have HIPAA-aware visibility into the conversations that move our Star Ratings.

The PHI redaction and member call screen recording won the day. Our compliance team signed off on the deployment in weeks, not quarters, and our competition said they just couldn't match Level AI on HIPAA-aware QA.

As a national health plan, member experience is everything we are measured on. Level AI's agent screen recording has added eyes to a process where we only had ears before. We can identify exactly where reps stumble on prior auth and formulary, coach them on member empathy, and watch our CAHPS-style scores climb.

We get so much intel about our member calls that it has reshaped how we run grievance and appeals. We've gone from manually scoring 1-2% of member calls to using Level AI to score 100% of them, and the operational signals we surface now reach the executive team weeks before they would have shown up in CMS data.

Level AI was the change we needed for member services. We doubled the productivity of our QA team, lifted member CSAT on appeals and benefits calls, and finally have HIPAA-aware visibility into the conversations that move our Star Ratings.

The PHI redaction and member call screen recording won the day. Our compliance team signed off on the deployment in weeks, not quarters, and our competition said they just couldn't match Level AI on HIPAA-aware QA.

As a national health plan, member experience is everything we are measured on. Level AI's agent screen recording has added eyes to a process where we only had ears before. We can identify exactly where reps stumble on prior auth and formulary, coach them on member empathy, and watch our CAHPS-style scores climb.

We get so much intel about our member calls that it has reshaped how we run grievance and appeals. We've gone from manually scoring 1-2% of member calls to using Level AI to score 100% of them, and the operational signals we surface now reach the executive team weeks before they would have shown up in CMS data.

A connected suite for health plan member services
HIPAA-aware context shared across QA, agent assist, voice of the member, and coaching, so benefits, formulary, prior auth, and appeals stay consistent on every member call.
AI Virtual Agent for Members
Resolve routine member calls without adding headcount. Handle ID card requests, PCP changes, formulary lookups, and benefits questions, then hand off to a licensed agent with full context for prior auth, appeals, and complex cases.

Auto-QA for Member Services
Every member call scored against your QA and CMS-aligned rubrics. PHI redaction in transcript and analytics, grievance precursor flags, and clear visibility into the calls sample-based QA misses.

Coaching on Member Empathy
Coaching built from real member conversations. Identify empathy gaps on appeals and benefits calls, surface where reps falter on formulary and prior auth, and track improvement that lifts CAHPS-style member experience scores.

Voice of the Member
See what members are saying at scale. Detect grievance themes, network-adequacy and access-to-care complaints, sentiment shifts on PA denials, and emerging Star Ratings risk across 100% of member interactions.

Member Operations Insights
A HIPAA-aware source of truth built from every member conversation. Turn unstructured calls into operations-ready insight on benefits confusion, formulary churn, network gaps, and the upstream signals that move Star Ratings.

Agent Assist for Benefits and PA
Real-time guidance for member services reps on benefits, formulary, prior auth, and appeals. Consistent with plan policy, network rules, and the member's coverage tier, surfaced the moment it is needed.
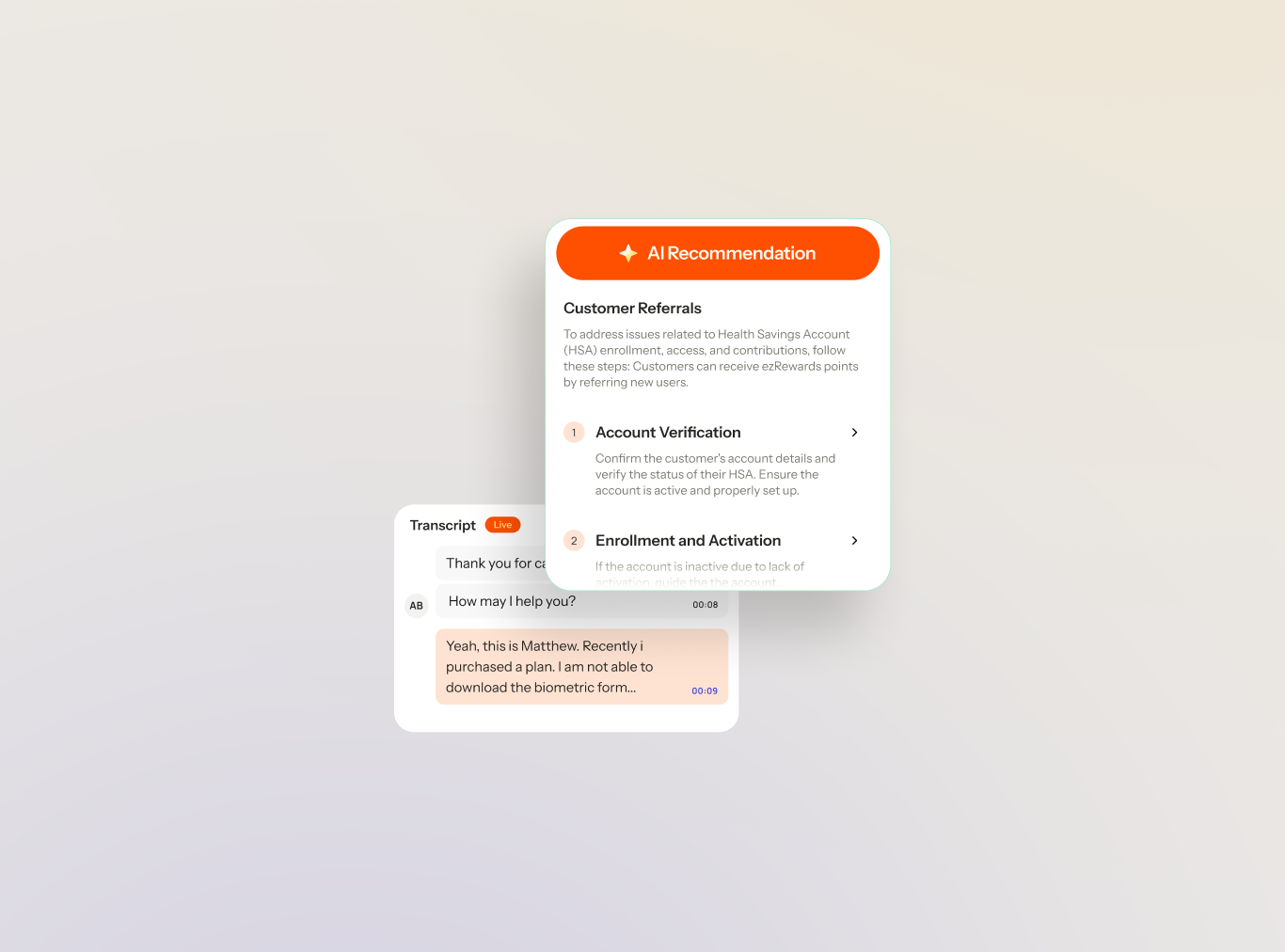
Measured impact for payers

Business Outcomes
Enhance CX and service quality with automated, impartial, and objective monitoring of every single customer interaction to your exact standards. Get deep insights into the drivers of CX across the organization. Learn how one of our customers saved over $30 million by leveraging Level AI's QA-GPT.
Scale your contact center to new heights by fully automating QA and call disposition, increasing first-call resolution with real-time assistance, and 5x faster targeted interaction reviews and coaching.
Increase revenue with real-time AI that identifies upsell opportunities, buyer reactions, and more to prompt the next best actions. Employ cutting-edge generative AI to proactively identify areas of product improvement.
Built for high-stakes customer experience
Trusted by teams that need accuracy, governance, and real outcomes across every customer touchpoint.
Built for every CX role
Streamline operations across all the areas of your contact center, from onboarding new support agents, coaching, managing team performance, identifying actionable insights for business growth, and more.
Learn moreSupercharge your performance with real-time AI guidance for the next best actions, instant post-call dispositions, contextual information from past calls and knowledgebases, and more.
Learn moreTurn your CX team from reactive to proactive with deep generative AI powered insights that get to the root cause and quantify even potentially unknown customer issues.
Learn more
More resources for CX teams

Frequently Asked Questions
Customer intelligence (CI) refers to the process of collecting, analyzing, and interpreting data about your customers to gain insights into their needs, preferences, and behaviors. This information can be used to improve various aspects of your business, such as marketing, product development, and customer service.
Personalize customer experiences: Tailor your offerings and interactions to individual needs.
Identify customer trends: Gain insights into emerging preferences and market shifts.
Improve product development: Create products and services that resonate with your target audience.
Boost customer satisfaction: Proactively address customer concerns and deliver exceptional service
Conversational intelligence is a subset of Customer Intelligence that focuses specifically on analyzing customer interactions through voice and text channels. This includes phone calls, live chats, emails, and social media messages.
Service automation refers to the use of technology to automate manual tasks traditionally performed by customer service agents. This can include tasks like:
- Real time AI assistance for agents
- Post call disposition
- Scoring agent performance in customer interactions
- Automated identification of unknown customer pain points
Level AI offers a suite of advanced artificial intelligence solutions, leveraging the latest generative AI and semantic intelligence technologies, that improve customer experience, greatly increase operational efficiency, and transform service & contact center teams into hubs of competitive advantage, insightful business intelligence, and growth.